Contact Us
1 Pickle Mews, London, SW9 0FJ
Virtual Reality in Healthcare: Why Clear Definitions Matter
Published
Jun 16, 2025
Tags
Virtual reality is transforming healthcare training, but without shared definitions, progress stalls. Learn why a common language in healthcare VR is essential for research, training, and real-world clinical impact.
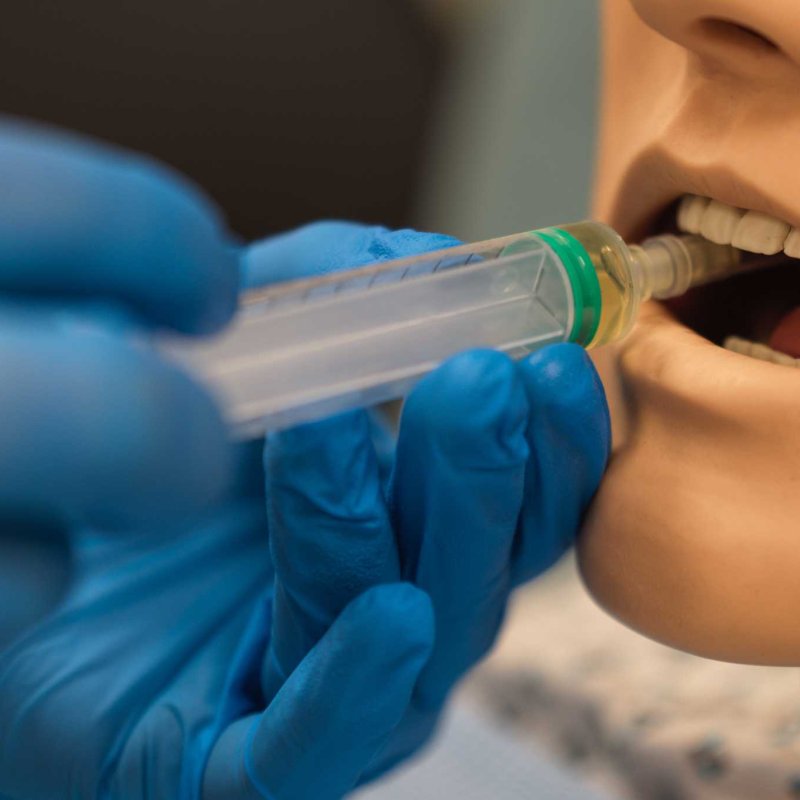
From immersive surgical training to primary care simulations, virtual reality (VR) is reshaping how we deliver care and train medical professionals. Yet, despite growing adoption rates, there's one foundational problem we keep running into: we’re not speaking the same language when discussing VR.
A published systematic review—co-authored by Jonathan Abbas, ExR’s co-founder, takes a critical look at this growing gap. The study analyses over 450 peer-reviewed papers in healthcare and uncovers widespread inconsistency in how VR is defined, described, and categorised. And it raises a crucial question:
If we can’t agree on what VR is, how can we accurately measure its value in healthcare?
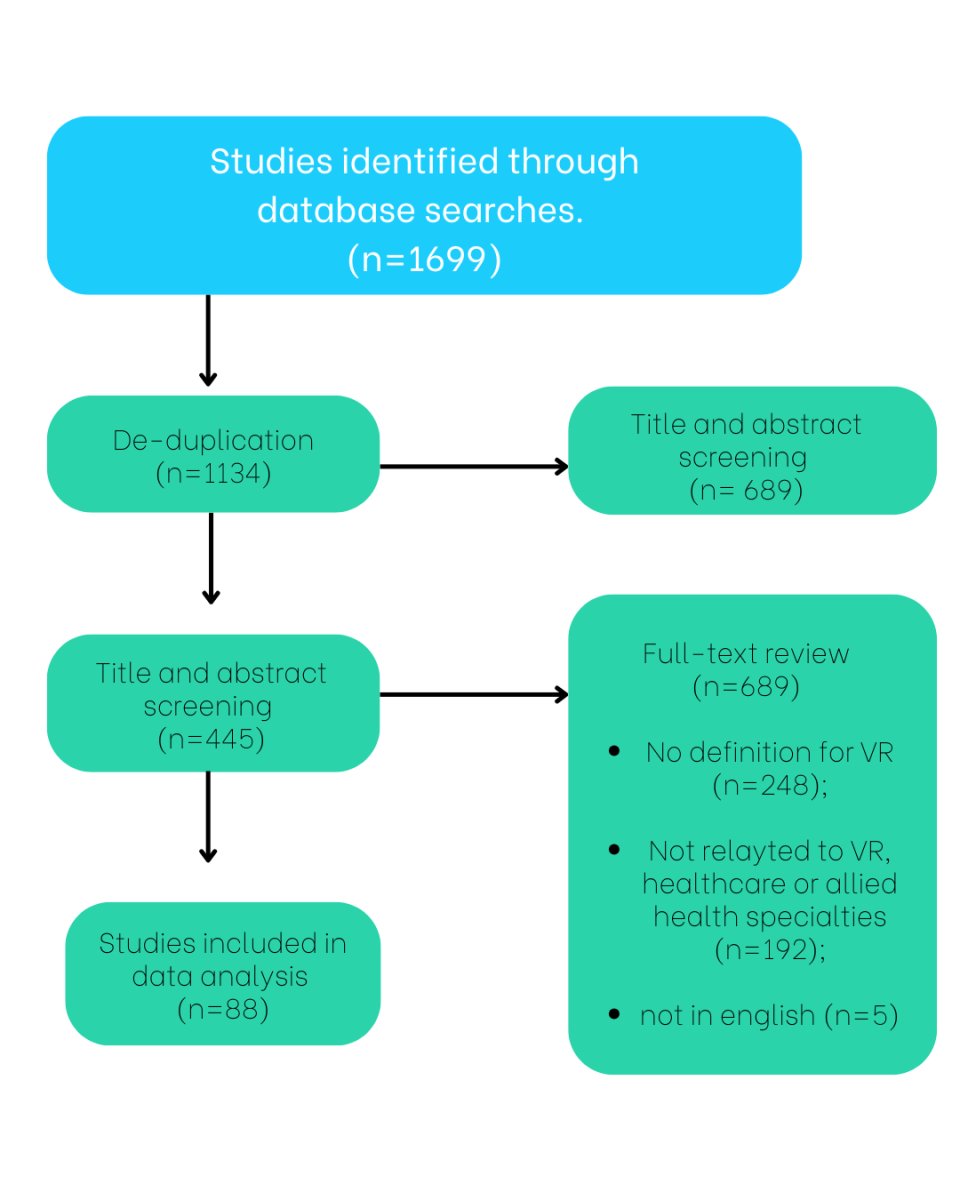
In the systematic review, a total of 1,688 articles were initially identified across three databases: Scopus (669 articles), PubMed/Medline (653 articles), and Web of Science (366 articles). After removing duplicates, 1,134 unique articles remained for screening. Following a review of titles and abstracts, 689 articles were excluded, resulting in 445 articles selected for full-text assessment.
Applying the predefined inclusion criteria, 357 articles were further excluded—248 for not providing a definition of VR, 192 for not addressing VR, and 5 for being non-English. Ultimately, 88 articles met the inclusion criteria by offering a definition of VR. The PRISMA flowchart illustrating the study selection process is presented below:
An Inconsistent Terminology Landscape
The term "Virtual Reality" is used liberally, but often imprecisely. Some researchers use it to describe fully immersive, interactive simulations rendered through head-mounted displays (HMDs). Others apply it to desktop-based environments or even simple 360° videos. As the review demonstrates, these inconsistent definitions have significant downstream effects—especially when it comes to interpreting research findings, scaling interventions, or securing regulatory approval.
This inconsistency becomes especially problematic in clinical contexts. Imagine evaluating the efficacy of “VR therapy” for anxiety. One study might use a passive 360° relaxation video on a tablet; another, a dynamic exposure environment with full interactivity. Without clarity, comparing those two outcomes is like comparing a flashlight to a laser—related, but not equivalent.
Definitions of VR Over Time
The definitions below have been cited more than once throughout the study.
First Author | Publication Year | Citation Frequency | Full Definition |
McCloy R | 2001 | 4 | “Virtual reality is best described as a collection of technologies that allow people to interact efficiently with 3D computerised databases in real time using their natural senses and skills.” |
Schultheis MT | 2019 | 3 | “VR can be viewed as an advanced form of human-computer interface that allows the user to "interact" with and become "immersed" in a computer-generated environment in a naturalistic fashion.” |
Park MJ | 2019 | 2 | “Virtual reality (VR) is defined as a computer-generated simulation, such as a set of images and sounds that represents a real place or situation, that can be interacted with, in a seemingly real or physical way by a person using special electronic equipment” |
Steuer J | 1992 | 2 | “Virtual reality is defined as a real or simulated environment in which a perceiver experiences telepresence” |
International Nursing Association of Clinical and Simulation Learning (INACSL) Standards Committee | 2016 | 2 | “A computer-generated reality, which allows a learner or group of learners to experience various auditory and visual stimuli. This reality can be experienced through the use of specialized ear and eyewear” |
Adamovich SV | 2009 | 2 | “Virtual reality (VR) can be defined as an approach to user-computer interface that involves real-time simulation of an environment, scenario or activity that allows for user interaction via multiple sensory channels” |
Székely G | 1999 | 2 | “present virtual objects or complete scenes to all human senses in a way identical to their natural counterpart” |
Merriam-Webster Dictionary | 1987 | 2 | “an artificial environment which is experienced through sensory stimuli (such as sights and sounds) provided by a computer and in which one's actions partially determine what happens in the environment” |
Oxford English Dictionary | 2014 | 2 | “The computer-generated simulation of a three-dimensional image or environment that can be interacted with in a seemingly real or physical way by a person using special electronic equipment, such as a helmet with a screen inside or gloves fitted with sensors.” |
The Importance of Definitions of VR in Healthcare
In fields such as entertainment or education, a certain degree of imprecision in language may be acceptable and not critically impact outcomes. But in healthcare, where decisions impact lives, ambiguity is a liability. Clinical interventions demand replicability, regulatory compliance, and rigorous evaluation. If researchers, developers, and providers aren’t using a shared language, evidence-based practice suffers.
This isn’t just a theoretical concern:
- Clinicians may misinterpret a study’s outcomes based on assumptions about VR technology.
- Researchers may draw misleading conclusions when aggregating results in reviews or meta-analyses.
- Developers may build tools that over promise or underdeliver because they’re not calibrated to clinical expectations.
- Patients may be offered treatments that differ in key aspects from those validated by research.
And as digital therapeutics, extended reality, and AI-integrated simulations expand, the problem will only worsen if left unaddressed.
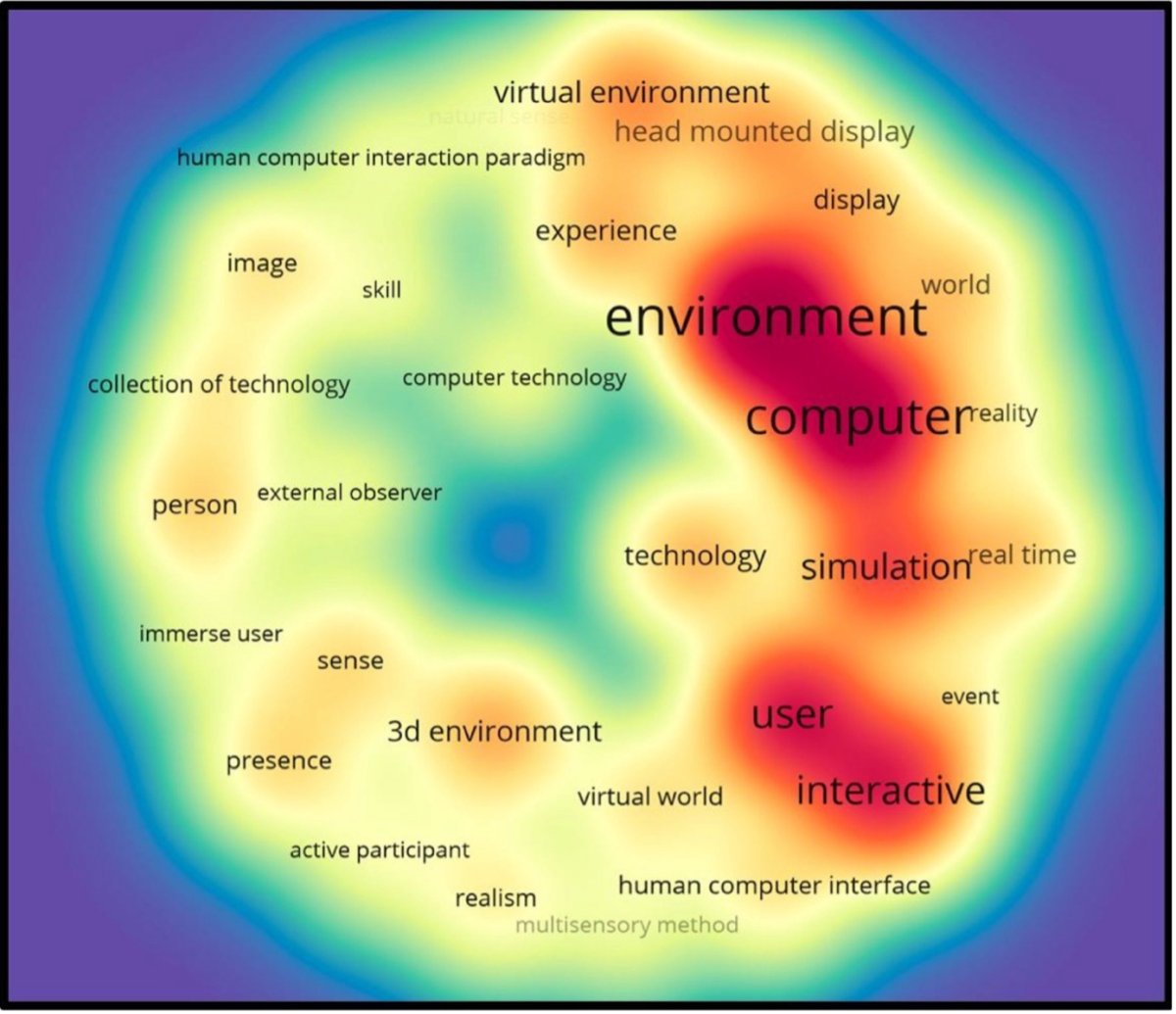
Discovered during the systematic review, there were 31 terms used when referring to VR. Below is a colour density map showing the most frequent terms (in red) and the less frequent terms (in blue).
From Confusion to Clarity: A New Typology for VR
The study offers a solution: a practical, flexible typology that defines VR systems based on three measurable dimensions:
- Immersion: Ranging from non-immersive (e.g. desktop environments) to fully immersive (e.g. HMD-based simulations). This dimension addresses how deeply a user is "placed" within the virtual world.
- Interactivity: Does the user merely watch, or can they manipulate and navigate the environment? This is crucial in differentiating passive viewing (like 360° videos) from true interactive VR.
- Sensory Complexity: This considers how many sensory channels are engaged. Does the experience include only visuals, or are there spatialised audio and haptic elements too?
By applying this framework, developers and researchers can more accurately describe their interventions. It also enables clinicians and regulators to assess tools based on clearly articulated features—not assumptions or marketing language.
Implications for Research, Practice, and Policy
Adopting this typology across healthcare could reshape how VR is understood and applied in real-world settings. Here’s how:
- Researchers can design and report studies with greater clarity, improving reproducibility.
- Clinicians can better assess which VR tools match their therapeutic goals.
- Developers can build solutions that align with clinical expectations and patient needs.
- Regulators and funders can evaluate interventions using standardised benchmarks.
What it Means for us at ExR: Building a Shared Language for Healthcare VR
At ExR, clarity isn’t just a design principle, it’s a foundation for clinical credibility.
In healthcare, language shapes understanding. When virtual reality is used to train future clinicians or support real-world medical procedures, the way we describe those experiences matters just as much as the technology itself. Ambiguity in simulation types or learning objectives doesn’t just slow innovation; it risks miscommunication in settings where precision is critical.
That’s why our work begins with clear definitions and ends with shared meaning.
Whether we’re developing a 360° knee replacement simulation with The Robert Jones and Agnes Hunt Orthopaedic Hospital or designing immersive placements for student nurses with the South Yorkshire Primary Care Workforce & Training Hub, we embed consistency and clarity into every stage, from co-creation with clinical teams to final deployment in training environments.
We believe that VR tools must speak the same language across geographies, departments, and disciplines. Without clear, consistent language, there’s a risk that tools designed for learning end up being interpreted or used differently than intended.
When terminology starts to align, so too does the potential for more meaningful collaboration, more consistent outcomes, and stronger evidence. Standardising how we describe VR in healthcare doesn’t just help scale solutions, it could help make them more trusted, more effective, and easier to measure.
By contributing to a unified framework for healthcare VR—both in how it works and how we talk about it—we’re helping set the stage for evidence-based, interoperable solutions that can support the future of medical education.
To advance the potential of immersive training, we must evolve not only the tools—but the terminology.
If you’d like to learn more about how ExR can help integrate immersive learning into your healthcare training strategy, get in touch with our team.
Most recent posts
Like what you read?
Please get in touch with us.