Contact Us
1 Pickle Mews, London, SW9 0FJ
The experiment
At Warwick Medical School in the United Kingdom, a small pilot study set out to see whether a low‑cost virtual‑reality (VR) training package could boost confidence and competence. Twenty third‑year medical students volunteered and were randomly split into two groups.
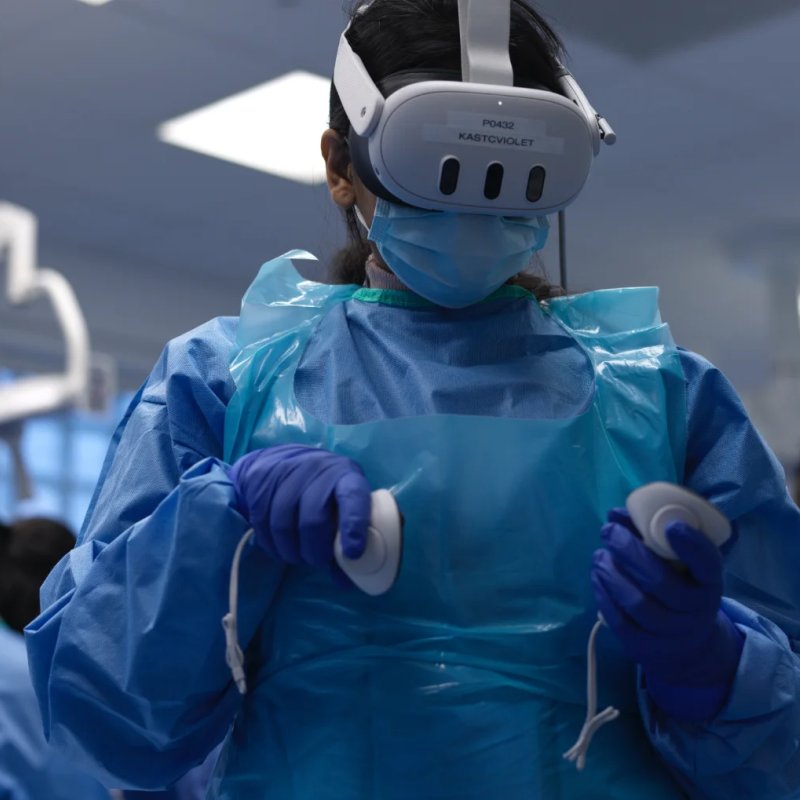
- VR group: Each participant wore an HTC Vive Focus 3 headset. Through three interactive platforms—Virti, 3D Organon, and ExR—they could explore a 3‑dimensional model of the throat, watch a 360‑degree video of the drainage technique, and practice the steps in a simulated environment.
- Traditional group: These students received a conventional 90‑minute lecture with static images and discussion.
Both groups completed the same pre‑session knowledge quiz, then after the teaching session they took a post‑session quiz and an Objective Structured Clinical Examination (OSCE), which is a hands‑on test of procedural skill.
What the results showed
The VR learners walked away with noticeably higher OSCE scores—averaging around 27 out of a possible 30—while the traditional group averaged about 21.5. This difference was statistically significant, indicating that the VR experience translated into better practical performance.
Beyond raw scores, the VR participants reported feeling more confident about performing the drainage, more engaged during the session, and generally more excited about the learning method. Their confidence ratings were significantly higher than those of the traditional group. Importantly, the VR group experienced almost no motion sickness; the average rating for cybersickness was just under two on a ten‑point scale.
Both groups improved substantially on the knowledge quizzes, but there was no meaningful difference between them after the session. In other words, VR didn’t give a huge advantage in pure factual recall, but it shone when it came to applying that knowledge in a simulated clinical setting.
Why this matters
- Confidence translates to safety – Students who feel ready are more likely to perform the procedure correctly when faced with a real patient.
- Risk‑free repetition – VR lets trainees practice the drainage step‑by‑step without any danger to patients, something hard to arrange in busy clinical settings.
- Cost‑effectiveness – After the initial purchase of headsets and software licenses, each additional training session adds little expense, making the model scalable for medical schools and hospitals.
- Higher engagement – The immersive experience captured attention and enthusiasm, potentially encouraging more students to explore ENT—a specialty that traditionally receives limited exposure.
Caveats
The study involved only twenty participants, so the findings need validation in larger cohorts. It also measured performance immediately after the training; we still don’t know how well the skills are retained weeks or months later. Finally, VR is a supplement, not a replacement, for real‑patient experience—hands‑on clinical work remains essential.
Looking forward
The researchers suggest a few next steps: comparing the same educational content delivered on a regular 2‑D screen versus in full VR to isolate the headset’s added value, conducting longer‑term follow‑ups to assess knowledge retention, and expanding the approach to other under‑taught procedures across medical specialties.
Where to read the full paper
The complete article is available on PubMed: McCormick M, Jegatheeswaran L, Homer‑Vanniasinkam S, Karamchandani D. “Virtual reality meets ENT: a low‑cost high‑fidelity teaching course for peritonsillar abscess drainage.” J Laryngol Otol 2025;1‑6. DOI 10.1017/S0022215125102983. You can access it here: https://pubmed.ncbi.nlm.nih.gov/40734282/
Try the EXR component yourself
The 360° EXR video that formed part of the VR curriculum is freely available to all NHS staff. You can explore the task directly at: https://app.exr.education/tasks/ee452348-245d-4099-862a-ad2a96621077/
Bottom line
A modest VR setup-combining interactive dialogue, 3‑D anatomy, and a free ExR video-helped medical students perform a critical throat drainage procedure more confidently and competently than a traditional lecture alone. As the technology becomes cheaper and more widely accessible, immersive VR could become a routine part of medical education, giving future clinicians a safe sandbox to rehearse lifesaving skills before they ever touch a real patient.
Most recent posts
Like what you read?
Please get in touch with us.