Contact Us
1 Pickle Mews, London, SW9 0FJ
From Headsets to Healing: How VR is Revolutionising Nose‑Packing Training for New Doctors
Published
Sep 09, 2025
Tags
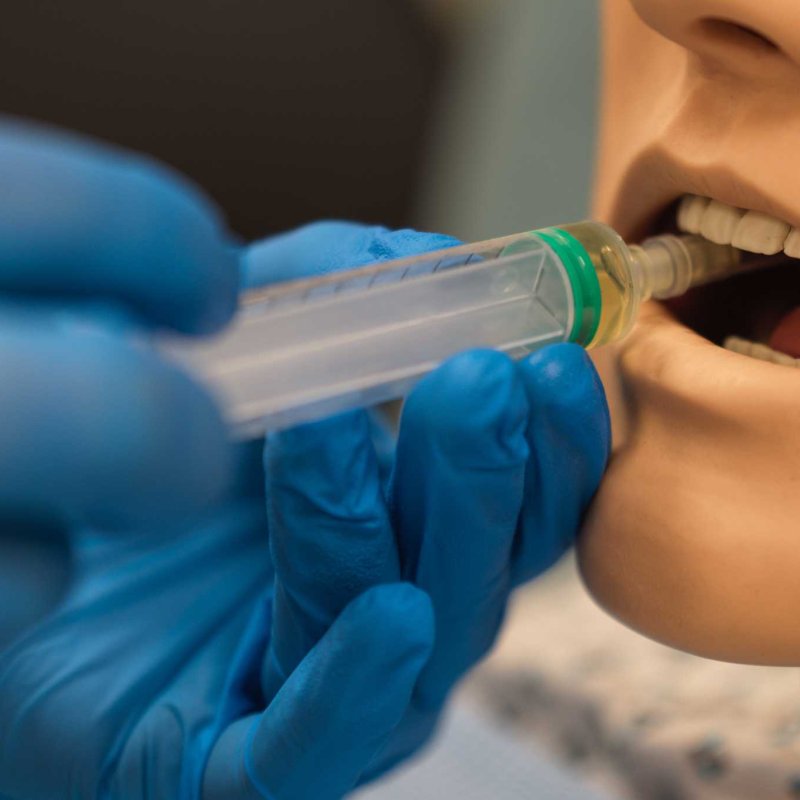
When a patient’s nose starts bleeding heavily—a condition known as epistaxis—the speed and accuracy of treatment can make all the difference. Yet many newly qualified doctors receive only a handful of hands‑on opportunities to practice this seemingly straightforward procedure before they are called upon to perform it in an emergency department.
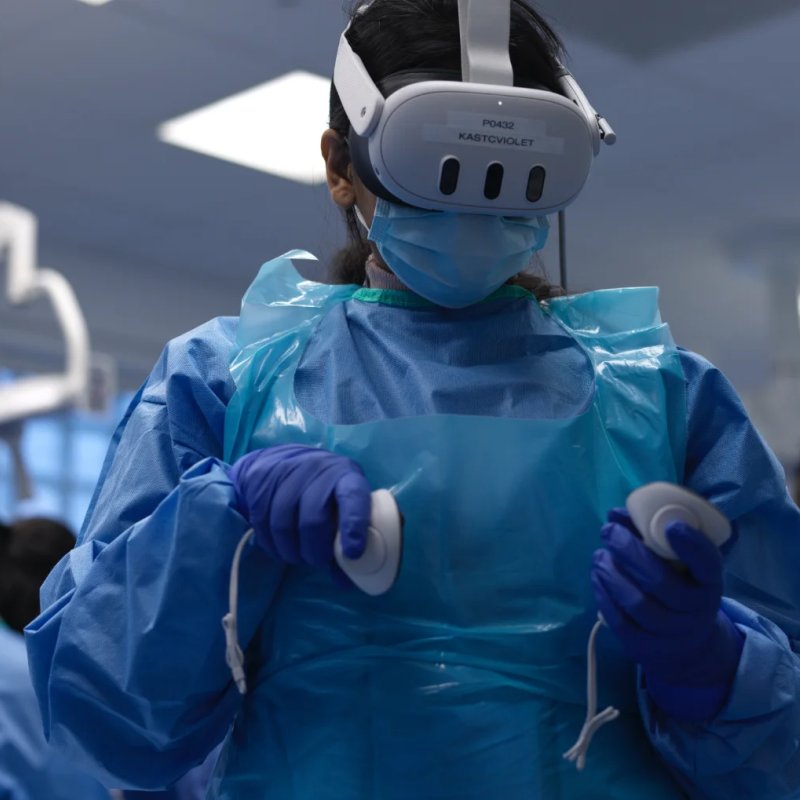
A recent UK study set out to see whether modern immersive technologies could bridge that gap. Sixteen foundation‑year doctors (the first two years after medical school) were invited to try three different learning experiences. One group used a fully immersive virtual‑reality (VR) simulator, another watched a 360° video of the procedure, and a third group experienced both in succession. Before and after each session the participants answered short questionnaires that measured how confident they felt, how competent they believed they were, and how many factual questions they could answer about the steps involved. They also rated how easy and enjoyable the tools were to use.
What the researchers found
Across all three groups, confidence rose dramatically—from a low rating of about two out of five before training to roughly four after. The sense of competence showed a similar jump, and knowledge scores on the quiz climbed from just over one point to more than four points out of five.
The 360° video consistently earned the highest usability scores, while the VR‑only experience lagged a bit behind. Both formats satisfied “content validity,” meaning they covered the essential steps accurately. The video also achieved full “face validity”—learners felt it looked and behaved like a real procedure. The VR simulation fell short mainly because its haptic (touch) feedback didn’t feel realistic enough; the sensation of actually packing the nose felt somewhat artificial.
Doctors’ impressions
Participants described the experience as fun and immersive, noting that the sense of being “inside” the procedure helped them concentrate. Some found the VR controllers fiddly, especially left‑handed users who struggled with a design geared toward right‑handed people. A spotty Wi‑Fi connection occasionally made the video appear blurry. Many suggested improvements such as a replay button, an “ask for help” cue, and a test mode that lets learners try the steps without prompts.
Beyond nasal packing, the doctors were eager to see the technology applied to other quick, step‑by‑step procedures—things like catheter insertion, lumbar puncture, or chest‑drain placement.
Why this matters to everyday readers
Even if you never step into an operating theatre, you rely on doctors to handle emergencies efficiently. Training that is engaging, repeatable, and low‑risk can translate into faster, safer care for patients. Here’s why the study’s findings are worth noting:
- Practice without risk – VR and 360° videos let trainees rehearse repeatedly without endangering anyone.
- Portable learning – Once the content is created, a headset or even a smartphone can deliver the lesson anywhere—hospital, classroom, or home.
- Instant feedback – Learners see right away where they excel and where they need improvement, speeding up skill acquisition.
- Scalable and affordable – Compared with building full‑size mannequins or organizing live workshops, digital modules can be shared widely at a fraction of the cost.
Looking ahead
The study was small and conducted at a single centre, so larger, multi‑site trials are needed to confirm the benefits and see whether the gains persist over months or years. The researchers also plan to upgrade the VR system’s tactile feedback—perhaps with more sophisticated gloves or force‑feedback devices—to make the “feel” match reality more closely.
For now, the message is clear: immersive technology is already proving its worth in medical education, especially for quick, high‑stakes procedures like anterior nasal packing. As these tools become more refined and widespread, patients can look forward to doctors who are not just knowledgeable on paper, but also confident and competent when the unexpected happens.
If you’re a medical student, a junior doctor, or simply curious about how tomorrow’s physicians will train, keep an eye on VR and 360° video platforms—they’re shaping the next generation of clinicians, one immersive experience at a time.
You can sign up and access this content for free here.
You can read the full paper here.
Most recent posts
Like what you read?
Please get in touch with us.